Key Takeaways:
-
Neurogenic bladder happens when nerve signals that control the bladder are disrupted. While there is no cure, it can be managed successfully.
-
Diabetes can damage bladder nerves, which can lead to neurogenic bladder. A 2023 review reports diabetes-related bladder dysfunction in 43-87% of people who have type 1 diabetes and 25% of people with type 2 diabetes.
-
If you have neurogenic bladder and experience urinary incontinence, you may qualify for free bladder control supplies, like pads or adult protective underwear, through Aeroflow Urology.
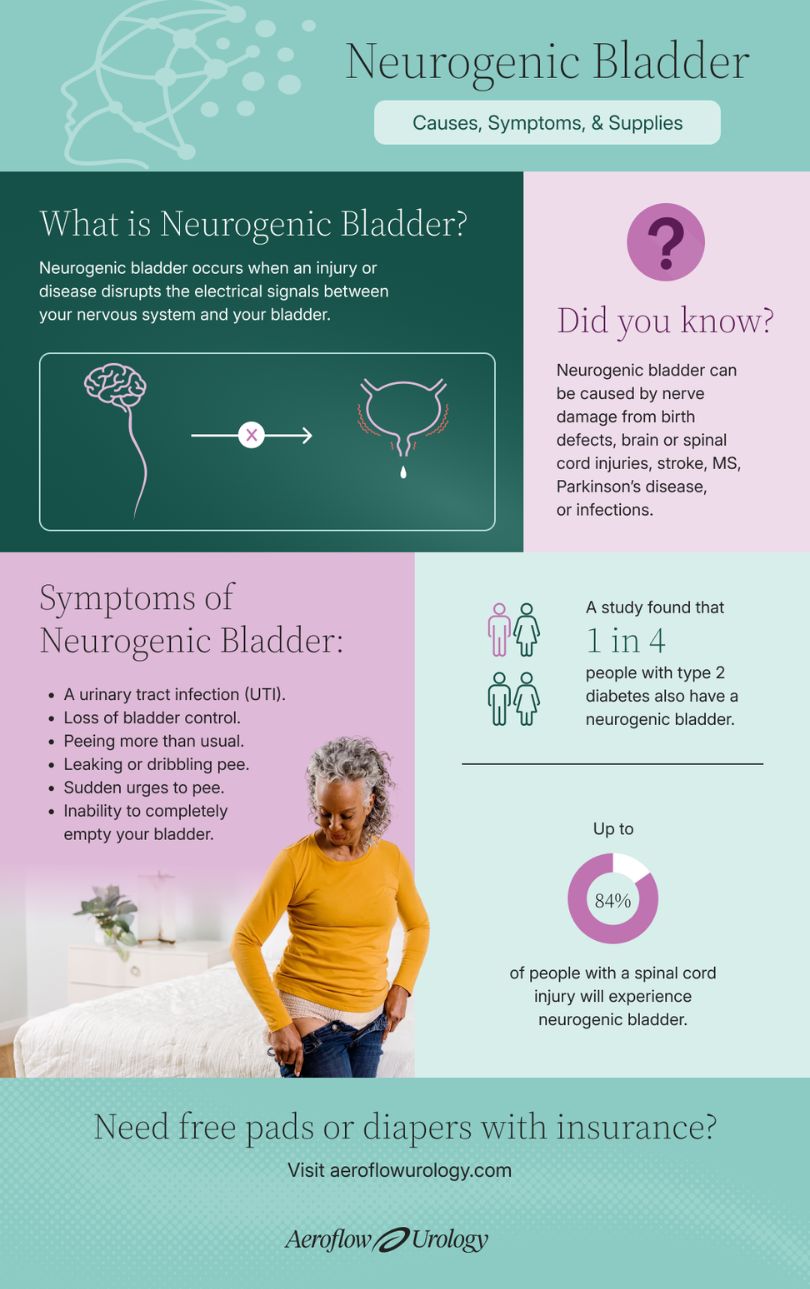
Neurogenic bladder occurs when an injury or disease disrupts the electrical signals between your brain, spinal cord, and bladder. Those nerves usually tell your bladder when to hold urine and when to release. However, when those messages get mixed up, you may begin experiencing leaks, a strong urge to pee, or feeling like you can’t fully empty your bladder.
Learn what causes neurogenic bladder, common symptoms, how it’s diagnosed, and treatment options your provider may recommend, such as using free, insurance-covered incontinence supplies like pads or diapers.
What Is Neurogenic Bladder?
Neurogenic bladder is the term for when nerve problems affect the way your bladder works. It is also referred to as neurogenic lower urinary tract dysfunction (NLUTD).
Your bladder functions through constant teamwork: nerves send messages between your brain and bladder muscles to help you store urine, then empty when you’re ready to urinate.
With neurogenic bladder, those messages don’t travel correctly. This can cause two main patterns:
-
Overactive bladder (OAB) signals: Your bladder squeezes too often, causing urgency and leaks. This is also known as a spastic or hyperflexive bladder.
-
Underactive bladder signals: Your bladder doesn’t squeeze enough, so you don’t empty fully (retention), which can lead to overflow leaks. This is also known as a flaccid or hypotonic bladder.
Some people can experience both an overactive and an underactive bladder.
What Causes Neurogenic Bladder?
Neurogenic bladder is usually linked to a condition or injury that affects your nervous system. Common causes include:
Congenital Conditions:
-
Caudal regression syndrome (also known as sacral agenesis).
Conditions From Illness, Injury, or Surgery:
-
Spinal cord injuries.
-
Traumatic injuries, such as a fall or a car accident.
-
Multiple sclerosis (MS).
-
Stroke
-
Brain or spinal cord tumors.
-
Severe infections that affect the nervous system (such as meningitis).
Experiencing bladder leaks? Check your coverage for $0 supplies!
Symptoms of Neurogenic Bladder
One of the most common signs that you may be experiencing neurogenic bladder is when you aren’t able to control when you pee. However, symptoms depend on the type of nerve damage you may have. Other symptoms may include:
-
Urinary tract infections (UTIs): A UTI can be a sign of neurogenic bladder. They can occur when a part of the urinary system becomes infected with bacteria, viruses, or yeast.
-
Leaks: Overflow leaks (when the bladder is too full) or even dribbling after you pee can be a symptom of neurogenic bladder. Leaks can also happen during the day or when you sleep.
-
Urgency and frequency: Strong, sudden urges to urinate, peeing often, or waking up at night to void may be a sign of neurogenic bladder.
-
Trouble emptying: Experiencing a weak stop-and-start stream, needing to strain, or feeling like you didn’t fully empty your bladder can be another symptom of neurogenic bladder.
Diagnosis and Testing
A healthcare provider will usually start by asking you about your medical history and your symptoms, then order bladder or nervous system tests.
If they recommend tests, they may include:
-
Urinalysis / urine culture: Checks for infection.
-
Bladder scan (post-void residual): Measures how much urine is left after you pee.
-
Cystoscopy: Used to look inside your urethra and bladder; sometimes ordered if a blockage or other bladder issue is suspected.
-
Urodynamic testing: Shows how your bladder stores and releases urine.
-
Imaging tests: If retention is a concern, your healthcare provider may request ultrasounds, X-rays, MRIs, or CT scans.
If you show signs of neurogenic bladder, they may refer you to a specialist, such as a urologist.
When should you see a healthcare provider?
Be upfront with your provider about any bladder control issues.
Visit a doctor right away if new symptoms develop or worsen, including if you have possible signs of an infection, such as pain or a fever.
If you are experiencing urine leakage, learn how to schedule a doctor’s appointment for incontinence.
Treatment Options for Neurogenic Bladder
Treatment depends on your symptoms, the cause, and your risk of complications. The main goal is to protect your kidney health, reduce infections, and make daily life easier.
Some treatment options for neurogenic bladder include:
-
Pelvic floor therapy: A trained physical therapist can teach you exercises and relaxation techniques to strengthen your pelvic floor muscles, which may help reduce leaks, urgency, and improve bladder control.
-
Bladder training: Once your provider says you can add bladder training to your routine, try habits like timed voiding. A schedule can help you with urge incontinence.
-
Medications: Several medications can help you treat neurogenic bladder, such as tolterodine, oxybutynin, mirabegron, vibegron, or tamsulosin. These medications are prescribed based on your symptoms, and are divided by anticholinergics (reduce bladder urgency), beta agonists (to relax the bladder), or alpha-blockers (to improve bladder emptying).
-
Bladder Botox: Your healthcare provider may inject Botox into your bladder or urinary sphincters to help you increase the amount of urine you can hold and reduce your symptoms of urgency and leakage.
-
Catheterization: If you are unable to empty your bladder, your doctor may recommend a urinary catheter. These can include a continuous catheter (wear at all times) or an intermittent catheter (single-use tubes)
-
Augmentation cystoplasty: This is a type of surgery meant to increase the size of your bladder so it can help you hold more pee.
-
Urinary reconstruction: A surgeon reroutes urine to a small opening on your belly (stoma). Your urine then drains into a bag worn outside your body (ostomy bag).
What is the best treatment for neurogenic bladder?
There isn’t a “best” or “first-line” treatment for neurogenic bladder, as what works best for you depends on your symptoms and the cause of your symptoms.
However, many healthcare providers start with simple, practical steps, such as using bladder control supplies like pads or absorbent underwear to help you stay dry and protect your skin. Access to free bladder control supplies can even reduce the risk of UTIs.
Experiencing bladder leaks? Check your coverage for $0 supplies!
Living With Neurogenic Bladder
Neurogenic bladder may feel frustrating, but a few simple habits can make your symptoms easier to manage and boost your confidence.
Practical tips that can help:
-
Establish a regular bladder schedule: Try timed voiding (peeing on a schedule) and set alarms on your phone.
-
Monitor your fluid intake: Drink enough water, but consider slowing down a few hours before bed if nighttime trips are a concern.
-
Limit bladder irritants: Avoiding common bladder triggers such as caffeine, alcohol, carbonated drinks, and spicy foods may prevent your bladder from becoming irritated.
-
Try Kegels: Kegels, a form of pelvic floor exercises, may help with improving your urinary leaks and urgency. These exercises may benefit men and women. Before you begin an exercise routine, check with your healthcare provider to see if they’re a good fit for you.
Frequently Asked Questions
Can neurogenic bladder be fixed or cured?
No, neurogenic bladder generally can’t be cured, but it can be highly manageable. With a proper diagnosis, treatment, and monitoring, many people can improve bladder control and prevent complications. In some cases, if the underlying neurological condition improves, bladder function may partially recover.
What happens if a neurogenic bladder is left untreated?
Neglecting to treat a neurogenic bladder can worsen your symptoms and increase your risk of infections. This can potentially lead to kidney damage, kidney failure, recurrent UTIs, bladder stones, chronic urinary retention, or even permanent loss of bladder function. Contact your doctor if you experience any symptoms of neurogenic bladder.
Which drug is used to treat neurogenic bladder?
A variety of medications can treat neurogenic bladder. Anticholinergics (such as oxybutynin or tolterodine) can reduce bladder overactivity, beta agonists (such as mirabegron or vibegron) can relax the bladder, and alpha blockers (like tamsulosin) can improve bladder emptying. The right medication depends on your symptoms and what your doctor recommends.
Can neurogenic bladder cause kidney problems?
Yes, if neurogenic bladder isn’t properly treated, urine can build up or the bladder can stay under high pressure, which may lead to complications over time, such as repeated infections or, in some cases, kidney damage.
Can lifestyle choices lead to neurogenic bladder?
Factors such as chronic alcohol use, leading a sedentary lifestyle, and not drinking enough water can raise your risk of nerve damage or worsen bladder dysfunction, which can lead to neurogenic bladder.
Is neurogenic bladder the same as overactive bladder?
No, an overactive bladder (sometimes called spastic neurogenic bladder) is a type of neurogenic bladder. Overactive bladder is a group of symptoms, such as sudden urgency and frequent urination, sometimes leakage, and it can occur with or without a neurologic condition.
References
Aleksandrov, A., Osorio, F., Khazali, S., Usta, T., Lemos, N., & Rabischong, B. (2025). Bladder dysfunction after advanced pelvic surgeries: Neuropelveological strategies for prevention and management. Facts, Views & Vision in ObGyn, 17(3), 271–280.
Elliott, C., Kreydin, E., Crew, J., & Shem, K. (2025). The current epidemiology of urinary incontinence and urinary tract infections after spinal cord injury—A Model Systems Spinal Cord Injury Examination (2016–2021). Journal of Clinical Medicine, 14(5), 1434.
Leslie, S. W., Tadi, P., & Tayyeb, M. (2023, July 4). Neurogenic bladder and neurogenic lower urinary tract dysfunction. In StatPearls. StatPearls Publishing.
Powell, C. R., & Gehring, V. (2023). Mechanisms of action for diabetic bladder dysfunction—State of the art. Current Bladder Dysfunction Reports, 18, 173–182.
Uren, A. D., & Drake, M. J. (2017). Definition and symptoms of underactive bladder. Investigative and Clinical Urology, 58(Suppl 2), S61–S67.
Disclaimer
Information provided on the Aeroflow Urology blog is not intended as a substitute for medical advice or care from a healthcare professional. Aeroflow recommends consulting your healthcare provider if you are experiencing medical issues relating to incontinence.